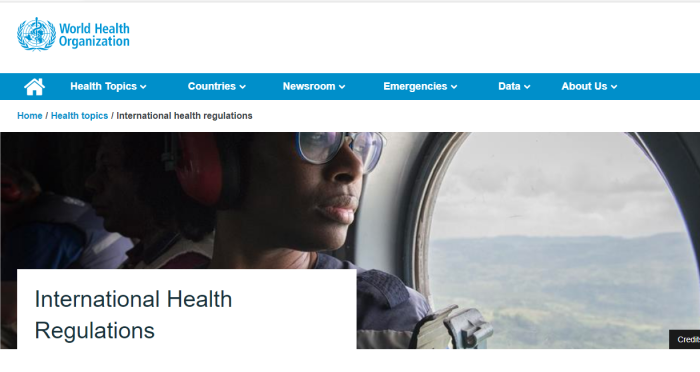
The IHR are an instrument of international law that is legally-binding on 196 countries, including the 194 WHO Member States. The IHR grew out of the response to deadly epidemics that once overran Europe. They create rights and obligations for countries, including the requirement to report public health events. The Regulations also outline the criteria to determine whether or not a particular event constitutes a “public health emergency of international concern”.
Canada has been following the legally binding dictates of the World Health Organization and their International Health Regulations. Let’s see what some of them are.
CLICK HERE, for International Health Regulations Archives.
CLICK HERE, for January 23 Statement from WHO.
https://archive.is/MapcO
CLICK HERE, for January 30 Statement from WHO.
https://archive.is/OjFyN
CLICK HERE, for May 1 IHR Statement from WHO.
https://archive.is/Y3pTe
CLICK HERE, for August 1 IHR Statement from WHO.
https://archive.is/JgR3A
CLICK HERE, for November 4, 2004 Quarantine Act hearings.
November 4 2004 Quarantine Act Evidence HESAEV06-E
quarantine.act.dec.8.2004.hearings
January 23 Statement (1st IHR Meeting)

To other countries
It is expected that further international exportation of cases may appear in any country. Thus, all countries should be prepared for containment, including active surveillance, early detection, isolation and case management, contact tracing and prevention of onward spread of 2019-nCoV infection, and to share full data with WHO.
Countries are required to share information with WHO according to the IHR.
Technical advice is available here. Countries should place particular emphasis on reducing human infection, prevention of secondary transmission and international spread and contributing to the international response though multi-sectoral communication and collaboration and active participation in increasing knowledge on the virus and the disease, as well as advancing research. Countries should also follow travel advice from WHO.
January 23, 2020 WHO/IHR Statement
January 30 Statement (2nd IHR Meeting)

To all countries
It is expected that further international exportation of cases may appear in any country. Thus, all countries should be prepared for containment, including active surveillance, early detection, isolation and case management, contact tracing and prevention of onward spread of 2019-nCoVinfection, and to share full data with WHO. Technical advice is available on the WHO website.
Countries are reminded that they are legally required to share information with WHO under the IHR.
Any detection of 2019-nCoV in an animal (including information about the species, diagnostic tests, and relevant epidemiological information) should be reported to the World Organization for Animal Health (OIE) as an emerging disease.
Countries should place particular emphasis on reducing human infection, prevention of secondary transmission and international spread, and contributing to the international response though multi-sectoral communication and collaboration and active participation in increasing knowledge on the virus and the disease, as well as advancing research.
The Committee does not recommend any travel or trade restriction based on the current information available.
Countries must inform WHO about travel measures taken, as required by the IHR. Countries are cautioned against actions that promote stigma or discrimination, in line with the principles of Article 3 of the IHR.
Under Article 43 of the IHR, States Parties implementing additional health measures that significantly interfere with international traffic (refusal of entry or departure of international travellers, baggage, cargo, containers, conveyances, goods, and the like, or their delay, for more than 24 hours) are obliged to send to WHO the public health rationale and justification within 48 hours of their implementation. WHO will review the justification and may request countries to reconsider their measures. WHO is required to share with other States Parties the information about measures and the justification received.
January 30, 2020 WHO/IHR Statement
May 1 Statement (3rd IHR Meeting)

The WHO Regional Emergency Directors and the Executive Director of the WHO Health Emergencies Programme (WHE) provided regional and the global situation overview. After ensuing discussion, the Committee unanimously agreed that the outbreak still constitutes a public health emergency of international concern (PHEIC) and offered advice to the Director-General.
The Director-General declared that the outbreak of COVID-19 continues to constitute a PHEIC. He accepted the advice of the Committee to WHO and issued the Committee’s advice to States Parties as Temporary Recommendations under the IHR.
The Emergency Committee will be reconvened within three months or earlier, at the discretion of the Director-General. The Director-General thanked the Committee for its work.
Risk communication and community engagement
Continue risk communications and community engagement activities through the WHO Information Network for Epidemics (EPI-WIN) and other platforms to counter rumours and misinformation.
.
Continue to regularly communicate clear messages, guidance, and advice about the evolution of the COVID-19 pandemic, how to reduce transmission, and save lives.
Travel and Trade
Continue working with countries and partners to enable essential travel needed for pandemic response, humanitarian relief, repatriation, and cargo operations.
.
Develop strategic guidance with partners for the gradual return to normal operations of passenger travel in a coordinated manner that provides appropriate protection when physical distancing is not feasible.
August 1 Statement (4th IHR Meeting)
After ensuing discussion, the Committee unanimously agreed that the pandemic still constitutes a public health emergency of international concern and offered advice to the Director-General.
.
The Director-General declared that the outbreak of COVID-19 continues to constitute a PHEIC. He accepted the advice of the Committee to WHO and issued the Committee’s advice to States Parties as Temporary Recommendations under the IHR (2005).
(6) Continue to work with partners to counter mis/disinformation and infodemics by developing and disseminating clear, tailored messaging on the COVID-19 pandemic and its effects; encourage and support individuals and communities to follow recommended public health and social measures.
(7) Support diagnostics, safe and effective therapeutics and vaccines’ rapid and transparent development (including in developing countries) and equitable access through the Access to COVID-19 Tools (ACT) Accelerator; support all countries to implement the necessary clinical trials and to prepare for the rollout of therapeutics and vaccines.
(8) Work with partners to revise WHO’s travel health guidance to reinforce evidence-informed measures consistent with the provisions of the IHR (2005) to avoid unnecessary interference with international travel; proactively and regularly share information on travel measures to support State Parties’ decision-making for resuming international travel.
August 1, 2020 WHO/IHR Statement
Quarantine Act Is Domestic IHR Implementation
Mr. Colin Carrie: Yes.
.
Are you aware of international standards for quarantine?
.
Dr. Paul Gully: The international health regulations would be the regulations that individual states would then use to design their quarantine acts. I don’t know of any other standards out there or best practices to look at quarantine acts, but the IHRs really have been used over the years as the starting point.
.
Now, with the improvement of the international health regulations, maybe, as is the case in Canada, changes will occur to quarantine acts in other countries in order to better comply with the international health regulations.
.
Mr. Colin Carrie: How is the communication now between different levels of government–for example, the federal government and the provinces–when something occurs?
.
(1140)
.
Dr. Paul Gully: The communication between the agency and the chief medical officers, for example, has always been good. The challenge during SARS was not necessarily the communication, but the information that was available to communicate.
.
The ability of Ontario to collect information, for example, to analyse it, and then for us to get it and to share it internationally was a challenge. That’s certainly something that Ontario and the Government of Canada have recognized, and as a result of that, other jurisdictions have recognized that as well.
.
We’ve certainly taken note of the lessons from SARS and the Naylor report. We’re always trying to improve that communication, but then, as I said, we are dependent on the abilities of other jurisdictions.
.
Mr. Colin Carrie: All right. I thought that was important, to see the different communications between each level, provincial and federal, but also international, because it seems that this is such a global thing right now.
Dr. Paul Gully: We had a meeting in September with the provinces and territories in Edmonton about the Quarantine Act as it stood at that time. We got input. We’re having another teleconference with the Council of Chief Medical Officers next week to talk about a number of issues that were raised and to further clarify what they would like to see as changes to the bill as it stands at the present time.
.
Mrs. Carol Skelton: Why did Health Canada proceed with a separate Quarantine Act at this time?
.
Dr. Paul Gully: Those of us who administered the Quarantine Act over the years always knew there were deficiencies in the old act, and because it was rarely used there wasn’t the inclination to update it. As a result of SARS and utilization of the act, which certainly put it under close scrutiny, and the requirement for the Government of Canada to respond to the various reports on SARS, it was felt that updating the act sooner rather than later was appropriate.
.
In addition, during discussions about the international health regulations of the World Health Organization, it was felt that it was appropriate to do it and to spend time and energy, which it obviously does require, to do it now, before other parts of legislative renewal, of which Mr. Simard is well aware, were further implemented or further discussion was carried out.
.
(1200)
Ms. Ruby Dhalla: I have one question. In terms of the Quarantine Act for our country, where are we at in terms of best practices models when we look at the international spectrum?
.
Dr. Paul Gully: I don’t know the acts in other countries, but because we are updating our act right now and we’re taking into account the probable revisions to the international health regulations, I believe we would be well in the forefront in terms of having modern legislation.
.
The Chair: Thank you.
.
Ms. Skelton.
.
Mrs. Carol Skelton: Following up on what Mr. Merrifield and Mr. Carrie said, it says in subclause 5(1) that the minister may “designate persons, or classes of persons, as analysts, screening officers or environmental health officers”. I think we should have in the act who those people are, so that they make sure they are trained professionals.
,
(1210)
.
Dr. Paul Gully: I believe that’s defined under the quarantine officer. At least in part, the quarantine officer refers to a medical practitioner or other health practitioner.
.
The reason for distinguishing between the three is that the screening officers would not require much training as the quarantine officers, as we defined. For an environmental officer, if it’s not defined, the implication is…. The quarantine officers are in subclause 5(2). I don’t believe, in fact, we’ve defined the qualifications of an environmental health officer, and maybe we should think about that. I think the term in this country, the use of the term “environmental health officer”, does imply some training, but I take your point.
https://www.ourcommons.ca/DocumentViewer/en/38-1/HESA/meeting-6/evidence
WHO Actually Governs Quarantines In Canada
Get it now? The 2005 Quarantine Act was Ottawa domestically implementing the latest edition of the International Health Regulations, or at least what what the changes were anticipated to be.
Restricting international travel (or not in this case), contact tracing, and efforts to shut down what they call “misinformation” are all done at the behest of the World Health Organization.
In fact, the Federal Government doesn’t run the show, nor do the Provinces. As part of our membership with WHO, Canada is legally obligated to follow the IHR.
